Rhinoplasty (nose surgery) Melbourne
Dr Rodrigo Teixeira (FRACS) is a Specialist Plastic Surgeon in Melbourne who performs primary rhinoplasty for cosmetic and functional concerns. Planning is tailored to your anatomy, diagnosis, and goals, with careful attention to proportion, structural support, and long-term stability as healing progresses.
Why Rhinoplasty May Be Considered?
Rhinoplasty, also referred to as nose job, may be considered to change the shape, proportion, or contour of the nose, and may address aesthetic concerns, breathing-related concerns, or both. Whatever the primary aim, preserving stable nasal support and function remains a key part of planning.
Breathing concerns are often present and may relate to structural factors such as septal deviation, weakness in nasal support, or narrowing of the nasal valves. Previous injury or trauma can also affect both appearance and airflow and may influence the surgical plan. When aesthetic and functional goals appear to conflict, decisions are guided by safety principles and long-term structural support.
Dr Rodrigo Teixeira is a Specialist Plastic Surgeon (FRACS) with a practice focus on facial plastic surgery, including rhinoplasty. His fellowship training includes aesthetic plastic surgery and craniofacial and cleft surgery, supporting an anatomy-led approach when planning nasal shape, support, and breathing considerations.

Learn more about Dr Rodrigo Teixeira and his approach to plastic surgery and patient care.
Concerns Addressed by Rhinoplasty
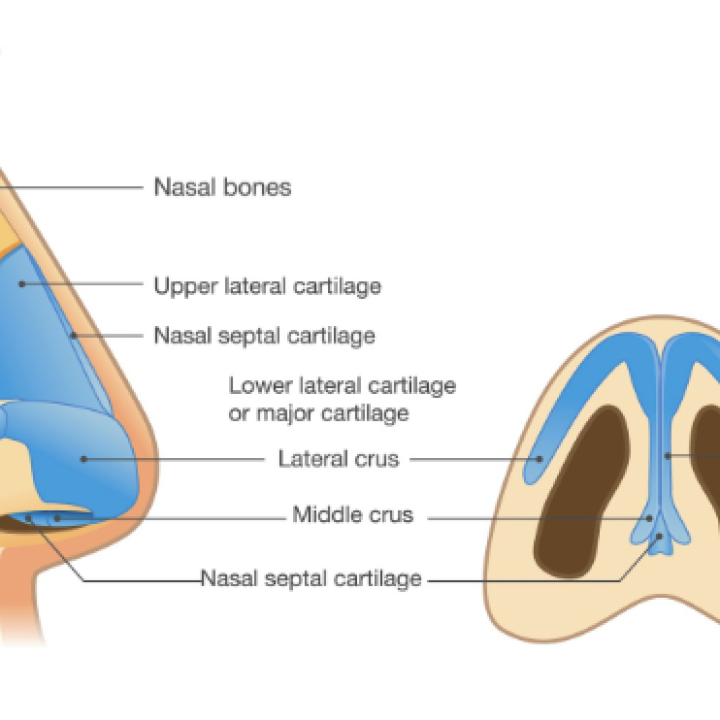
Many nasal concerns are surface expressions of deeper anatomy. Bone and cartilage provide structural support, the septum and internal valves influence airflow, and the skin–soft tissue envelope affects contour and definition. Each of these elements may contribute independently or in combination, which is why rhinoplasty begins with anatomical diagnosis rather than treating a visible feature in isolation.
Not all noses have the same structure, and not every concern is aesthetic alone. Dorsal shape, tip support, septal alignment, skin thickness, facial proportions, and breathing function all need to be assessed before deciding whether rhinoplasty is appropriate, or whether a different or additional procedure may be considered.
Refining a Dorsal Hump or Nasal Prominence
A dorsal hump may involve bone, cartilage, or a combination of both. In some patients, the concern is not only the height of the bridge, but also how it relates to tip position, radix height, and overall facial balance. Rhinoplasty may improve dorsal contour by reshaping the underlying framework rather than treating the bridge as an isolated feature.
Improving Tip Shape and Definition
Nasal tip concerns may include a rounded tip, reduced definition, excessive width, asymmetry, or a tip that appears heavy or poorly supported. These features may relate to cartilage shape, projection, rotation, skin thickness, and structural support. In suitable patients, rhinoplasty may improve tip contour through careful modification and support of the lower nasal cartilages.
Addressing a Drooping or Underprojected Nasal Tip
Tip position can influence both nasal shape and facial proportions. A drooping tip may become more noticeable on smiling or in profile view, while an underprojected tip may reduce definition and support. Rhinoplasty may improve this by adjusting projection, rotation, and support, depending on the underlying anatomy.
Straightening a Crooked or Deviated Nose
A crooked nose may reflect asymmetry of the nasal bones, septal deviation, cartilage irregularity, or a combination of structural factors. In some patients, the concern is primarily visual, while in others it may also be associated with breathing difficulty. Rhinoplasty may improve nasal alignment (nose realignment), though residual asymmetry can remain and depends on the underlying anatomy.
Nostril Width and Flare
In some patients, the appearance of a wider nose relates to the nostril base (the alar region). Alar base reduction may be discussed to address nostril width or flare as part of overall rhinoplasty planning. Any trade-offs, such as scar placement, symmetry limitations, and how small changes can alter overall nasal balance, are reviewed carefully during consultation.
Improving Nasal Breathing and Structural Support
Some patients seek rhinoplasty because of both appearance and function. Breathing concerns may relate to septal deviation, internal or external valve narrowing, prior injury, or weakness in structural support. Where airflow is affected, rhinoplasty may need to address both cosmetic and functional anatomy as part of the surgical plan.
Correcting Irregularities Following Injury or Previous Surgery
Changes in nasal shape may also occur after trauma or previous nasal surgery. These concerns can include contour irregularities, asymmetry, collapse, loss of support, or altered breathing. In these situations, treatment planning often requires more detailed assessment of scar tissue, cartilage support, and the relationship between form and function.
Surgical Approach in Primary Rhinoplasty
Nose surgery may be performed using different surgical approaches depending on the anatomy, the changes required, and the level of access needed to the nasal framework. This may include open or closed rhinoplasty, as well as preservation or more structural techniques where appropriate.
An open approach is commonly used where direct visibility of the bone and cartilage framework supports careful modification, structural grafting, or more detailed tip work. In selected cases, preservation principles may be incorporated to maintain key support structures and minimise unnecessary disruption. Where appropriate, ultrasonic surgery technique may also be used for bony reshaping in specific anatomical situations.
Planning Your Rhinoplasty
Rhinoplasty planning is tailored to the individual and begins with careful assessment of nasal anatomy, skin thickness, structural support, facial proportions, symmetry, and breathing function. The aim is not simply to change one feature, but to understand how the nose relates to the rest of the face and how any change may affect both appearance and function over time.
Planning may involve cosmetic concerns, functional concerns, or both. Common issues include a dorsal hump, a crooked nose, tip droop, under-projection, asymmetry, septal deviation, valve narrowing, or weakness in nasal support. Previous filler, prior surgery, or cleft-related differences may also influence what is appropriate and how surgery is planned.
Cosmetic Rhinoplasty
Cosmetic rhinoplasty focuses on refining nasal shape and proportion in a way that is appropriate to the individual face. Common concerns include a dorsal hump, a crooked nose, tip droop, under-projection, asymmetry, or a nose that appears out of balance with other facial features.
In planning, these concerns are not assessed in isolation. Bridge height, tip position, rotation, projection, skin thickness, and structural support may all influence the surgical plan. The aim is to make careful, balanced changes that respect both form and function while maintaining support for longer-term stability.
Functional Rhinoplasty and Septoplasty
Functional considerations are often assessed alongside cosmetic goals, particularly where there are concerns about nasal airflow. Common structural contributors include septal deviation, narrowing of the internal or external nasal valves, and weakness in nasal support.
Where appropriate, septal surgery may be performed to improve airflow. In some cases, the septum may also be used as a source of cartilage grafts for structural support. In others, it may not need to be approached at all. This depends on the anatomy, the surgical priorities, and whether the main issue is cosmetic, functional, or both. Learn more about septoplasty during rhinoplasty (rhinoseptoplasty).
Rhinoplasty After Non-Surgical Nose Reshaping
Some patients seek surgical rhinoplasty after previous non-surgical nose reshaping with filler. Prior filler may affect assessment and planning by altering tissue feel, contour, and the ability to evaluate the underlying framework accurately. For this reason, dissolving filler is often recommended before surgery is considered. Timing, safety, and whether this is appropriate are discussed during consultation, based on the individual anatomy and treatment history.
Other Related Nasal Procedures:
Revision rhinoplasty –Assessment after previous nasal surgery, where scar tissue, altered support, and healing limitations may increase complexity.
Cleft rhinoplasty – Assessment and surgical planning for cleft-related nasal differences, often with particular attention to asymmetry, support, and reconstructive considerations.
What to Expect During the Consultation
Your consultation focuses on understanding your concerns and assessing whether rhinoplasty is appropriate for your anatomy, goals, and nasal function. This includes review of relevant medical and nasal history, including previous injury, surgery, or non-surgical treatments, along with assessment of nasal shape, structural support, and breathing. The discussion also covers what may be achievable, what may be limited, and whether surgery is the most appropriate option.
Where helpful, clinical photography and optional imaging may be used to support communication during planning. These tools can help clarify priorities, but they do not predict exact outcomes and results vary between individuals. The consultation also includes discussion of the likely surgical approach, recovery, risks, and limitations. If surgery is not advised, this will be discussed openly, and where relevant, alternative options may be considered.
In younger patients, suitability is assessed with particular attention to facial growth, maturity, and emotional readiness. Cosmetic surgery in patients under 18 is also subject to additional safeguards under Australian guidelines.

Risks and Considerations
Like all surgical procedures, rhinoplasty carries potential risks and possible complications. These vary depending on your anatomy, medical history, skin and cartilage characteristics, healing response, and the extent of surgery performed. Because healing cannot be fully predicted, both aesthetic and functional outcomes may change over time, and specific results cannot be guaranteed.
General Surgical Risks
General surgical risks may include bleeding, infection, scarring, and risks related to anaesthesia. Although uncommon, these risks are recognised in rhinoplasty and are discussed during consultation along with the measures used to reduce risk.
Changes in Shape, Symmetry, and Surface Contour
As healing progresses, contour irregularities, asymmetry, or small differences in surface smoothness may become apparent. These may involve the bridge, tip, sidewalls, or areas where cartilage support has been altered. In some cases, concerns such as residual prominence, palpable irregularity, or recurrence of deviation may persist after healing.
Internal Scarring and Structural Healing
Healing inside the nose can also affect outcome. Internal scar formation or adhesions may influence airflow or, less commonly, contribute to changes in internal contour. Where grafts are used, there is also a small risk of warping, resorption, or shift during healing, which may affect support or shape over time.
Changes in Sensation and Visible Scarring
Temporary numbness or altered skin sensation can occur after rhinoplasty, and in some cases may persist for longer than expected. In open rhinoplasty, there is also a small external scar across the columella, which usually matures over time, although scar quality varies between individuals.
Breathing and Functional Complications
Because rhinoplasty changes nasal structure, breathing function must always be considered alongside appearance. Persistent obstruction, reduced airflow, or other functional concerns may arise due to swelling, septal position, internal valve compromise, scar formation, or changes in structural support. These concerns require careful reassessment.
When Further Treatment May Be Considered
In some cases, further treatment may be discussed if concerns persist after healing. This may involve observation, non-surgical management, a minor corrective procedure, or revision rhinoplasty, depending on the nature of the concern and reassessment of both nasal form and function.
Recovery and Aftercare
Recovery after rhinoplasty varies between individuals and depends on anatomy, the surgical plan, and how the tissues heal. Early changes are usually visible within the first few weeks, but refinement continues gradually as the nose settles. For more detail on rhinoplasty swelling and healing timelines, see our recovery blog here.
Early Recovery
For most patients, the most noticeable swelling and bruising occur in the first one to two weeks after surgery. This is often the period when time away from work or social commitments may be considered, depending on the type of work involved and individual comfort.
Returning to Activity
Return to activity is usually gradual. Light daily activity is often resumed first, while heavier exercise, lifting, and any activity that carries a risk of nasal impact may need to wait longer. Exact timing depends on the procedure performed and individual healing progress.
Swelling and Ongoing Refinement
Early swelling usually improves first, while more subtle swelling, particularly through the tip, may take much longer to resolve. This can affect how definition appears during different stages of recovery.
When Results Begin to Look More Settled
Many patients notice that the nose appears more settled after the early recovery period, but final refinement often continues over 12 to 18 months, and sometimes longer. This is influenced by factors such as skin thickness, scar response, and the extent of structural change performed during surgery.
Follow-Up and Aftercare
Specific aftercare instructions are provided after surgery, and follow-up appointments are used to monitor healing and address concerns at an appropriate stage of recovery.
Our Clinic in Ivanhoe East, Melbourne
Unveil Aesthetics and Plastic Surgery is located in Ivanhoe East, around 10 kilometres from Melbourne’s CBD. Our clinic on Lower Heidelberg Road is easily accessed, with convenient parking nearby, and provides a calm, welcoming environment designed for comfort and discretion.
When you arrive, our reception team will assist with check-in and help coordinate your appointment. We focus on clear communication, clinical professionalism, and coordinated follow-up throughout your care.
Choosing rhinoplasty is a significant decision. Our team aims to provide clear information, careful coordination, and continuity of care from consultation through recovery.
FAQs about Rhinoplasty
Most patients are advised to avoid resting glasses on the bridge of the nose for around 6 weeks, or until cleared at follow-up and it’s not painful. If needed, contact lenses or taping glasses to the forehead can reduce pressure on the nose during early healing.
Swelling settles gradually. Many patients feel the nose looks mostly settled by ~6 weeks, but fine swelling can continue to improve for 12-18 months, depending on anatomy and healing.
Most patients plan for around 10–14 days away from work and social commitments, as this is when swelling and bruising are often most noticeable. The timing can vary depending on your role, how you heal, and how comfortable you feel being seen during early recovery. Your surgeon will guide you based on your progress at follow-up appointments.
Exercise is usually resumed gradually. As a general guide, light cardio may be possible from around 2 weeks if healing is progressing as expected. Heavier lifting is typically reintroduced gradually from around 4 weeks, and contact sports are commonly avoided until around 8 weeks due to the risk of nasal impact. Exact timing can vary, so follow your surgeon’s instructions and your individual recovery plan.
Rhinoplasty may improve breathing when symptoms are related to structural factors such as a deviated septum or narrowing/weakness of the nasal valves. Not all breathing concerns are caused by nasal structure, so assessment is important to clarify what is contributing and whether surgical treatment is likely to help. If septal surgery is being considered as part of rhinoplasty planning, this will be discussed during consultation.
Open rhinoplasty uses a small incision at the base of the nose (on the columella) in addition to internal incisions, which can allow direct visibility of the nasal framework during surgery. Closed rhinoplasty is performed through incisions inside the nostrils only. Each approach has advantages and limitations, and the most appropriate option depends on the changes being considered, the support required, and individual anatomy. Your surgeon will explain which approach may be recommended in your case and why.
All surgery heals with some degree of scarring, but how noticeable scars become varies between individuals. Scar quality is influenced by factors such as skin type, healing response, and aftercare. Incision lines usually soften and fade over time, but scar appearance cannot be fully predicted. Your surgeon will discuss incision placement, scar care, and follow-up to support optimal healing.
The cost of rhinoplasty varies because it depends on the complexity of surgery, whether functional work (such as addressing breathing-related structural issues) is being considered, and the costs associated with the operating theatre, anaesthesia, and postoperative care. Fees can also differ based on surgical time, individual anatomy, and the level of aftercare required. For these reasons, an accurate estimate is usually provided after consultation, once a surgical plan is confirmed and you’re given a clear breakdown of what is included.
Hilotherm is a temperature-controlled cooling system that uses a soft, water-circulating mask to deliver consistent cooling (rather than ice packs that warm quickly). After rhinoplasty, it may be used in the early recovery period to support comfort and help manage swelling and bruising, following your surgeon’s instructions.